
A cervicogenic headache is head pain that originates from problems in your neck, specifically the upper cervical spine (C1-C3 vertebrae). Unlike migraines or tension headaches, this secondary headache develops when misaligned vertebrae, damaged discs, or stressed muscles irritate nerves that connect your neck to your head.
Treatment through upper cervical chiropractic care can reduce these headaches by addressing the root cause in your spine.
Key Facts
- Affects: 15-20% of all chronic headache sufferers; approximately 2-4% of the general population
- Primary Cause: 70% originate from the C2-C3 vertebral joint dysfunction
- Gender Distribution: Women are affected 4 times more frequently than men
- Age of Onset: Typically begins in early 30s; average age of diagnosis is 49
- Treatment Success: Spinal manipulation can reduce headache frequency by 50% or more
- Specialist: Upper cervical chiropractor, such as a Blair technique practitioner
Medical Disclaimer: This content is for informational purposes only and does not constitute medical advice. The information provided should not be used for diagnosing or treating health problems or diseases. Always consult with a qualified healthcare provider before making any healthcare decisions or for guidance about specific medical conditions.
What Is a Cervicogenic Headache?
A cervicogenic headache is a type of secondary headache that originates from disorders in your cervical spine—the upper portion of your neck.
Unlike primary headaches such as migraines or tension headaches that begin in the brain, cervicogenic headaches are caused by problems in the bones, discs, muscles, nerves, or soft tissues of your neck.
The term "cervicogenic" literally means "arising from the cervical spine." When structures in your upper neck become damaged, misaligned, or inflamed, they can irritate the nerves that transmit pain signals to your head.
This creates what doctors call referred pain, you feel the headache in your head, but the actual source of the problem is in your neck.
The International Headache Society officially recognizes cervicogenic headache as a distinct diagnosis with specific criteria. Norwegian physician Dr. Ottar Sjaastad first coined this term in 1983 after observing patients with chronic headaches that were clearly linked to neck problems.
Today, the Blair Chiropractic Technique and other upper cervical methods focus specifically on correcting the spinal misalignments that cause these headaches.
What Causes Cervicogenic Headaches?
Understanding the underlying cause of your cervicogenic headache is essential for effective treatment. Research shows that approximately 70% of cervicogenic headaches originate from dysfunction of the C2-C3 zygapophyseal joint—the small joints between the second and third cervical vertebrae.
The upper cervical spine (C1-C3) plays a critical role because nerves from this region connect directly to the trigeminocervical nucleus, a pain-processing center that receives signals from both your neck and your head.
Common Causes Include:
Upper Cervical Misalignment (Subluxation): When the atlas (C1) or axis (C2) vertebrae shift out of their proper position, they can compress nerves and blood vessels, triggering headache pain
Whiplash Injuries: Car accidents or sports injuries that jolt the neck can damage ligaments, muscles, and joints, leading to chronic cervicogenic headaches
Poor Posture ("Tech Neck"): Prolonged forward head position while using phones, computers, or tablets increases stress on upper cervical structures
Cervical Disc Degeneration: Age-related wear on spinal discs can irritate nerves and cause referred head pain
Arthritis: Osteoarthritis or rheumatoid arthritis affecting the cervical spine can inflame joints and compress nerves
Muscle Tension and Trigger Points: Chronic tightness in neck and shoulder muscles, often associated with stress or repetitive strain
Previous Head or Neck Trauma: Falls, sports concussions, or birth trauma can create lasting structural problems
Dr. Vladimir Janda identified a common pattern called Upper Crossed Syndrome in cervicogenic headache patients, characterized by tight muscles in the back of the neck and chest combined with weak muscles in the front of the neck and upper back.
This muscle imbalance pulls the head forward and increases strain on the upper cervical spine.
Signs and Symptoms of Cervicogenic Headaches
Cervicogenic headaches have distinctive characteristics that differentiate them from migraines and tension headaches. Recognizing these specific symptoms can help you and your healthcare provider determine if your neck is the true source of your head pain.
Primary Symptoms:
One-sided (unilateral) headache: Pain typically stays on one side and does not switch sides
Pain that starts in the neck: Headache originates at the base of the skull and radiates forward to the forehead, temple, or behind the eye
Reduced neck mobility: Difficulty or pain when turning or tilting your head
Headache triggered by neck movement: Certain head positions or sustained postures provoke or worsen pain
Tender spots in the neck: Pressing on specific points in your neck reproduces or intensifies headache pain
Steady, non-throbbing pain: Unlike migraines, the pain is typically dull and constant rather than pulsating
Additional Symptoms May Include:
- Neck stiffness and muscle tightness
- Shoulder or arm pain on the same side as the headache
- Blurred vision or difficulty focusing
- Dizziness or lightheadedness
- Sensitivity to light and sound (less common than with migraines)
- Nausea (rare compared to migraines)
Symptoms often worsen with prolonged static positions—such as working at a computer, driving, or sleeping in an awkward position. Many patients report that their headaches are worst in the morning or after periods of sustained neck strain.
SEEK IMMEDIATE MEDICAL ATTENTION IF YOU EXPERIENCE:
- Sudden, severe headache ("worst headache of your life")
- Headache with fever, stiff neck, and rash
- Neurological symptoms: sudden numbness, weakness, difficulty speaking, or vision loss
- Headache following head trauma or injury
- Headache with loss of consciousness or seizures
These symptoms may indicate a serious medical emergency such as stroke, meningitis, or brain hemorrhage. Call 911 or go to your nearest emergency room immediately.
How Is a Cervicogenic Headache Diagnosed?
Diagnosing cervicogenic headaches can be challenging because symptoms often overlap with migraines and tension headaches. A thorough evaluation by a qualified healthcare provider is essential for accurate diagnosis and effective treatment.
Diagnostic Process:
1. Comprehensive Health History: Your provider will ask detailed questions about your headache patterns, triggers, previous injuries, and medical history. Information about headache location, duration, and what makes symptoms better or worse helps distinguish cervicogenic headaches from other types.
2. Physical Examination: A hands-on assessment evaluates your neck range of motion, identifies tender points, and checks for muscle tightness. The Cervical Flexion-Rotation Test has high accuracy (91% sensitivity, 90% specificity) for detecting upper cervical dysfunction.
3. Neurological Evaluation: Testing reflexes, muscle strength, and sensation helps rule out more serious neurological conditions.
4. Diagnostic Imaging: X-rays, CT scans, or MRI may be ordered to visualize cervical spine structures. Blair upper cervical chiropractors use specialized 3D imaging to precisely identify misalignments that standard imaging may miss.
5. Diagnostic Nerve Blocks: In some cases, injecting local anesthetic into specific cervical nerves can confirm the diagnosis. If the headache temporarily disappears after the block, it strongly suggests a cervicogenic origin.
The International Classification of Headache Disorders (ICHD-3) requires clinical evidence of a neck disorder plus either clinical signs implicating a cervical source or abolition of headache following diagnostic nerve blocks.
Treatment Options for Cervicogenic Headaches
Effective treatment for cervicogenic headaches addresses the underlying neck problem rather than simply masking symptoms with medication. Research supports a multimodal approach combining manual therapy, therapeutic exercise, and lifestyle modifications.
Blair Upper Cervical Chiropractic Care
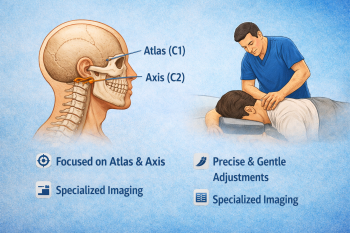
The Blair Chiropractic Technique is a specialized upper cervical approach that focuses precisely on the atlas (C1) and axis (C2) vertebrae—the primary sources of cervicogenic headaches. Unlike general chiropractic methods, Blair practitioners use:
Precision 3D Imaging: Detailed X-rays map your unique spinal anatomy to identify exact misalignments
Gentle, Specific Adjustments: No twisting, cracking, or popping—corrections are delivered with precise, controlled force
Individualized Treatment: Each adjustment is customized to your specific anatomy and misalignment pattern
Long-Lasting Results: Properly performed corrections can hold for weeks, months, or even years
Research published in evidence-based guidelines confirms that chiropractic care, including spinal manipulation, improves cervicogenic headaches. Studies show spinal manipulation can reduce headache frequency by approximately 50%, with benefits maintained at long-term follow-up.
Living With Cervicogenic Headaches
Managing cervicogenic headaches effectively involves combining professional treatment with daily self-care practices. While upper cervical chiropractic care addresses the root cause, lifestyle modifications can significantly reduce headache frequency and intensity between visits.
Daily Management Strategies:
- Maintain Good Posture: Keep your ears aligned over your shoulders. Avoid forward head position, especially when using devices
- Take Regular Breaks: If you work at a computer, stand and move every 30-45 minutes to prevent sustained neck strain
- Optimize Your Sleep Position: Use a supportive pillow that maintains neutral neck alignment. Avoid sleeping on your stomach
- Apply Heat or Cold: Heat can relax tight muscles; cold can reduce inflammation. Experiment to see which works best for you
- Practice Gentle Stretching: Regular neck stretches can improve flexibility and reduce muscle tension
- Manage Stress: Stress often triggers muscle tension that worsens cervicogenic headaches. Consider relaxation techniques like deep breathing or meditation
- Track Your Triggers: Keep a headache diary noting activities, positions, and situations that precede your headaches
Many patients develop "pattern recognition" for signs that their spine needs attention—such as feeling their head is heavy, noticing muscle tightness, experiencing brain fog, or observing postural changes. Working with a Blair chiropractor helps you understand your body's signals and maintain optimal spinal alignment.
Prevention Strategies
While not all cervicogenic headaches can be prevented, many cases can be avoided or significantly reduced through proactive measures that protect your cervical spine.
Key Prevention Measures:
- Ergonomic Workstation Setup: Position your computer monitor at eye level, keep your keyboard at elbow height, and ensure your chair provides proper lumbar support
- Strengthen Your Neck Muscles: Regular exercises targeting deep neck flexors improve stability and reduce strain on cervical joints
- Practice Proper Lifting Technique: Avoid straining your neck when lifting heavy objects; keep the load close to your body
- Wear Seatbelts Properly: Correct seatbelt positioning helps prevent whiplash injuries in motor vehicle accidents
- Limit Screen Time: Reduce prolonged use of phones and tablets that encourage forward head posture
- Regular Chiropractic Check-ups: Preventive spinal evaluations can identify and correct misalignments before they cause symptoms
Research suggests that lifestyle factors like prolonged sitting, repetitive neck movements, and poor posture have contributed to increased cervicogenic headache rates in recent years. Taking proactive steps to protect your neck health is more important than ever in our device-dependent world.
When to See a Doctor
Knowing when to seek professional evaluation for your headaches can prevent unnecessary suffering and ensure timely treatment. While occasional mild headaches may not require immediate attention, certain patterns and symptoms warrant professional assessment.
Schedule an Appointment If:
- Headaches occur more than twice per week
- Over-the-counter medications no longer provide relief
- Headache patterns have changed or worsened
- Neck pain or stiffness accompanies your headaches
- Headaches interfere with work, sleep, or daily activities
- You've experienced recent neck injury or trauma
- Headaches began after starting a new job or activity with different posture demands
- You're using pain medication more than 2-3 days per week
Early intervention is important because untreated cervicogenic headaches tend to become chronic and more difficult to manage over time. The longer abnormal spinal mechanics persist, the more compensatory changes develop throughout the spine.
Frequently Asked Questions
How do I know if my headache is coming from my neck?
Cervicogenic headaches typically start at the base of the skull and radiate to the front of the head, often staying on one side. Key indicators include reduced neck mobility, pain triggered by neck movements or sustained positions, and tender spots in your neck that reproduce headache pain when pressed.
If your headache responds to neck treatment but not to typical migraine medications, it likely has a cervical origin. A qualified healthcare provider can perform specific tests, like the Cervical Flexion-Rotation Test, to help confirm the diagnosis.
Can cervicogenic headaches be cured?
Many patients experience significant long-term relief or complete resolution of cervicogenic headaches with proper treatment. Upper cervical chiropractic care addresses the underlying spinal dysfunction that causes these headaches.
However, outcomes depend on factors including how long you've had the condition, the severity of structural changes, and your commitment to lifestyle modifications. Some patients require periodic maintenance care to maintain spinal alignment, while others hold their corrections for extended periods.
How long does it take for cervicogenic headaches to improve with chiropractic care?
Most patients begin noticing improvement within 2-8 weeks of starting Blair upper cervical care, though individual responses vary. Research indicates that 6-8 sessions of spinal manipulation produce favorable outcomes for cervicogenic headaches.
Chronic cases that have persisted for years may take longer to fully stabilize. Your chiropractor will monitor your progress and adjust your treatment plan based on how you respond.
Is the Blair chiropractic adjustment safe?
The Blair technique is considered very safe because it uses gentle, precise corrections without the twisting, cracking, or forceful manipulation associated with some other chiropractic methods.
Research shows that adverse events from spinal manipulation for headaches are few, mild, and transient, typically limited to temporary soreness or tiredness. The Blair technique is suitable for patients of all ages, including those who may be sensitive to more aggressive treatments.
What's the difference between cervicogenic headaches and migraines?
While both can cause significant head pain, they have different origins and characteristics. Migraines are primary headaches originating in the brain, often characterized by throbbing pain, nausea, and sensitivity to light and sound.
Cervicogenic headaches are secondary headaches caused by neck problems, typically presenting as steady (non-throbbing) pain that starts in the neck and radiates forward. Migraines may occur on either side and can switch sides, while cervicogenic headaches usually stay on one side. Some patients have both conditions, which can complicate diagnosis.
Can poor posture really cause headaches?
Yes, poor posture is a significant contributor to cervicogenic headaches. Forward head posture—increasingly common due to smartphone and computer use—places excessive stress on the upper cervical spine. For every inch your head moves forward, it effectively adds 10 pounds of weight that your neck muscles must support. This strain can lead to muscle imbalances, joint dysfunction, and nerve irritation that trigger headache pain. Correcting posture and addressing the resulting spinal misalignments are essential components of treatment.
How often will I need to see a chiropractor?
Treatment frequency varies based on your individual condition. Initially, you may need more frequent visits (typically 1-2 times per week) to establish correction and allow your spine to stabilize. As your condition improves, visits typically decrease to once every 4-6 weeks for maintenance. One advantage of Blair upper cervical care is that properly delivered adjustments often hold for weeks, months, or even years, requiring fewer total visits compared to other approaches.
Do I Need to See a Doctor? Quick Assessment
Answer these questions honestly about your current symptoms:
- Have your headaches persisted for more than 2 weeks without improvement?
- Do your headaches begin in your neck or base of skull?
- Is your neck range of motion limited or painful?
- Are your headaches triggered or worsened by neck movements or positions?
- Have over-the-counter pain medications become ineffective?
- Are headaches interfering with daily activities, work, or sleep?
- Have you experienced a neck injury, whiplash, or concussion?
- Do you spend extended periods looking at screens or in poor posture?
Your Results:
0-1 "Yes" answers: Continue monitoring symptoms and practicing self-care measures. Schedule a routine appointment if symptoms persist beyond 2-3 weeks.
2-3 "Yes" answers: Professional evaluation recommended. Schedule an appointment within 1-2 weeks to prevent worsening.
4-5 "Yes" answers: Prompt medical attention needed. Schedule an appointment within 2-3 days. Your symptoms indicate significant cervical involvement.
6+ "Yes" answers: URGENT evaluation needed. Contact a healthcare provider TODAY for same-day or next-day assessment.
Any red flag symptoms (sudden severe headache, neurological changes, fever with stiff neck): Seek IMMEDIATE emergency care.
Ready to Take the Next Step? Contact Dennis Campbell, DC at our Wasco, California office to schedule your comprehensive upper cervical evaluation. We specialize in Blair Chiropractic Technique for lasting headache relief.
Remember: When in doubt, seek professional advice. It's always better to be evaluated and reassured than to ignore symptoms that need attention.
Cervicogenic headaches are a distinct and treatable form of head pain that originates from problems in your upper cervical spine.
Unlike migraines or tension headaches, these secondary headaches respond best to treatment that addresses their root cause—misalignments, muscle imbalances, and dysfunction in the C1-C3 vertebral region.
The Blair Chiropractic Technique offers a precise, gentle approach specifically designed to correct upper cervical misalignments without the twisting or cracking associated with traditional chiropractic methods. Research supports the effectiveness of spinal manipulation for cervicogenic headaches, with many patients experiencing significant reduction in headache frequency and intensity.
If you've been struggling with headaches that seem connected to your neck, haven't responded to typical headache treatments, or developed after an injury, cervicogenic headache may be the explanation. A thorough evaluation by an upper cervical specialist can determine if your pain is coming from your neck and create a personalized treatment plan to address it.
Don't accept chronic headaches as a normal part of life. With proper diagnosis and targeted treatment, most people with cervicogenic headaches can achieve lasting relief and improved quality of life.
Main Points
- Cervicogenic headaches originate from the cervical spine, particularly the C1-C3 vertebrae, and cause referred pain to the head
- 70% of cases involve the C2-C3 joint, making upper cervical care particularly effective
- Spinal manipulation can reduce headache frequency by 50% or more according to research
- Blair Chiropractic Technique uses gentle, precise adjustments without twisting or cracking
- Early intervention prevents chronic patterns—don't wait for headaches to become severe or constant
References
Bryans R, et al. (2011). Evidence-based guidelines for the chiropractic treatment of adults with headache. Journal of Manipulative and Physiological Therapeutics, 34(5):274-89.
Chaibi A, et al. (2017). Chiropractic spinal manipulative therapy for cervicogenic headache: a single-blinded, placebo, randomized controlled trial. BMC Research Notes, 10:310.
Cleveland Clinic. (2024). Cervicogenic Headache: What It Is, Symptoms & Treatment. https://my.clevelandclinic.org/health/diseases/cervicogenic-headache
Haas M, et al. (2010). Dose response and efficacy of spinal manipulation for chronic cervicogenic headache: a pilot randomized controlled trial. The Spine Journal, 10:117-128.
International Headache Society. (2018). The International Classification of Headache Disorders, 3rd edition. Cephalalgia, 38(1):1-211.
Jull G, et al. (2002). A randomized controlled trial of exercise and manipulative therapy for cervicogenic headache. Spine, 27(17):1835-43.
National Center for Biotechnology Information. (2022). Cervicogenic Headache - StatPearls. https://www.ncbi.nlm.nih.gov/books/NBK507862/
Page P. (2011). Cervicogenic headaches: an evidence-led approach to clinical management. International Journal of Sports Physical Therapy, 6(3):254-66.
Robinson CL, et al. (2025). Prevalence and relative frequency of cervicogenic headache in population- and clinic-based studies: A systematic review and meta-analysis. Cephalalgia, 45(3).
Xu L, et al. (2023). Global trends in research on cervicogenic headache: a bibliometric analysis. Frontiers in Neurology, 14:1169477.
American Migraine Foundation. (2016). Cervicogenic Headache. https://americanmigrainefoundation.org/resource-library/cervicogenic-headache/
Blair Chiropractic Society. (2024). The Blair Technique. https://www.blairtechnique.com/the-blair-technique/
_______________________________________________
Last medically reviewed: November 2025
Dennis Campbell, DC | Blair Upper Cervical Chiropractic | Wasco, California





Leave a comment