
Waking up with back pain is common, but it is not always caused by one single problem.
In many cases, morning back pain happens because the body has stayed in one position for hours, joints and soft tissues become stiff overnight, or the spine is being stressed by poor sleep posture, an unsupportive mattress, muscle strain, or underlying inflammation.
Persistent morning stiffness that improves once you start moving can sometimes point to inflammatory conditions such as ankylosing spondylitis, while pain linked to lifting, posture, strain, or disc irritation is often mechanical in nature.
Why back pain feels worse when you first wake up
During sleep, your body is at rest for several hours. That sounds restorative, but long periods of stillness can also allow muscles, fascia, and spinal joints to tighten up.
If the tissues around the spine are already irritated, sleeping in one position too long may increase stiffness and discomfort by morning. Research on waking spinal symptoms also suggests that sleep posture can influence how the neck and back feel on waking.
For some people, the problem is mostly mechanical. Muscles may stay guarded after a day of sitting, lifting, commuting, or repetitive stress. The mattress or pillow setup may not support neutral spinal alignment well.
A stomach-sleeping position, for example, can place stress on both the neck and lower back. For others, the issue is more inflammatory, especially if the pain comes with prolonged morning stiffness, night pain, or improvement after movement rather than rest.
Common causes of morning back pain
One of the most common causes is muscle and ligament strain. A busy day, awkward lifting, exercise overload, or prolonged sitting can leave the back irritated.
You may not feel the full effect until the next morning, when the tissues have stiffened overnight. Back pain can also come from disc irritation, arthritis, sciatica, or general joint stress in the spine.
Poor sleep posture is another major contributor. If your body is twisted, overarched, or unsupported for hours, the spine may not get a real chance to recover.
Sleep systems matter too. A mattress that is too soft, too firm, or too worn out can place the body in a position that increases strain rather than reducing it.
Inflammatory conditions deserve attention as well. Ankylosing spondylitis, for example, is known for causing back pain and stiffness that are often worse in the morning and at night, and that tend to improve with exercise rather than rest.
When morning back pain regularly lasts more than 30 minutes, returns night after night, or is paired with alternating buttock pain, it should not be ignored.
Stress, poor sleep quality, fatigue, and long-term tension can also amplify pain sensitivity. Sometimes the back is not “injured” in a dramatic way, but the system is overloaded and less resilient, making morning symptoms more noticeable.
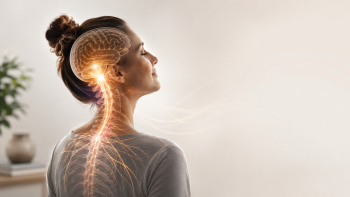
Where upper cervical chiropractic fits into the conversation
At first glance, morning back pain sounds like a lower back issue only. But the spine works as a connected system, not as isolated sections. Changes in posture and alignment in one region can influence mechanics elsewhere.
Evidence on spinal alignment and regional interdependence supports the idea that cervical posture can affect overall spinal balance and that problems in one region may contribute to strain in another.
That does not mean every case of morning back pain starts in the upper cervical spine. It means that in some patients, tension patterns, head and neck posture, sleep positioning, and whole-spine compensation may be part of the picture.
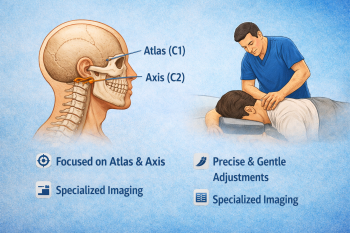
Upper cervical chiropractic focuses on the relationship between the head, neck, and nervous system, with the goal of improving balance and reducing abnormal mechanical stress.
In a patient who wakes with both neck tension and back stiffness, evaluating the upper cervical region may be clinically relevant as part of a broader structural assessment.
This whole-spine view can be especially valuable when morning pain keeps returning even after stretching, changing mattresses, or treating the lower back alone.
Signs your morning back pain may need professional evaluation
Occasional stiffness that eases quickly is common. Persistent or worsening pain is different. It is wise to seek evaluation if:
- stiffness lasts longer than 30 minutes most mornings
- pain wakes you during the night
- symptoms improve with movement but worsen with rest
- pain travels into the leg, or there is numbness or tingling
- symptoms follow injury, fever, unexplained weight loss, or significant weakness
These features can point to nerve irritation, inflammatory conditions, or other problems that need a proper diagnosis rather than guesswork.
What can help reduce back pain in the morning
The first step is identifying whether the pain is mostly mechanical, inflammatory, or related to sleep setup and daily habits.
For many people, simple changes help: better sleep posture, a more supportive pillow or mattress, gentle mobility on waking, regular movement breaks during the day, and avoiding prolonged static postures.
An office-worker trial found that active breaks and postural shifts reduced new neck and low back pain, reinforcing how much prolonged positioning can matter.
Heat may help with stiffness, and many cases of common back pain improve with conservative care rather than bed rest. Clinical guidance also favors movement and noninvasive care over prolonged inactivity.
When structural imbalance is part of the pattern, chiropractic evaluation may help determine whether spinal mechanics, posture, or upper cervical dysfunction are contributing factors.
In an upper cervical practice, that means looking beyond where the pain is felt and considering how the body is compensating as a whole.
Final thoughts
Morning back pain is often a message, not just a symptom. It may reflect overnight stiffness, poor sleeping mechanics, muscle strain, disc or joint irritation, or inflammation. In some cases, the problem is local to the lower back.
In others, the issue involves broader postural patterns and whole-spine compensation, including the upper cervical region.
For patients who keep waking up stiff, achy, or bent over until they get moving, it makes sense to look deeper. A careful assessment can help determine whether the issue is mechanical, inflammatory, or related to spinal balance and nervous system stress.
From an upper cervical chiropractic perspective, that broader view matters, because lasting relief often starts with understanding the full pattern, not just the place that hurts.
Throughout Wasco, Bakersfield, Shafter, Delano, Visalia, Fresno, and nearby San Joaquin Valley communities, many patients are searching for a more precise and measured approach to chiropractic care.
Upper cervical chiropractic offers that difference through focused analysis, gentle correction, and an emphasis on long-term structural balance.
Dr. Campbell’s professional, detail-oriented approach and welcoming office setting have made this practice a trusted destination for Blair Upper Cervical care.
Whether patients have been seeking this specific method for years or are exploring upper cervical chiropractic for the first time, they can expect care that is calm, intentional, and designed around individualized needs.
Browse the website to learn more about Blair Upper Cervical chiropractic and how the technique works. When ready, call the office to schedule an appointment and begin the process of restoring structural balance and supporting long-term health.
References
Mayo Clinic. Back pain: Symptoms and causes.
NHS. Back pain.
Park SC, et al. Assessment and nonsurgical management of low back pain. PMC.
NHS. Ankylosing spondylitis symptoms.
South & West Devon Formulary. Inflammatory back pain.
Cary D, et al. Examining relationships between sleep posture and waking spinal symptoms. PMC.
McDevitt A, et al. Regional interdependence and manual therapy. PMC.
Konishi T, et al. Effect of cervical flexion and extension on thoracic sagittal alignment. PubMed.
Lee SH, et al. Cervical sagittal alignment review. PMC.





Leave a comment